"We are running out of time. We have to prepare as many people as possible"
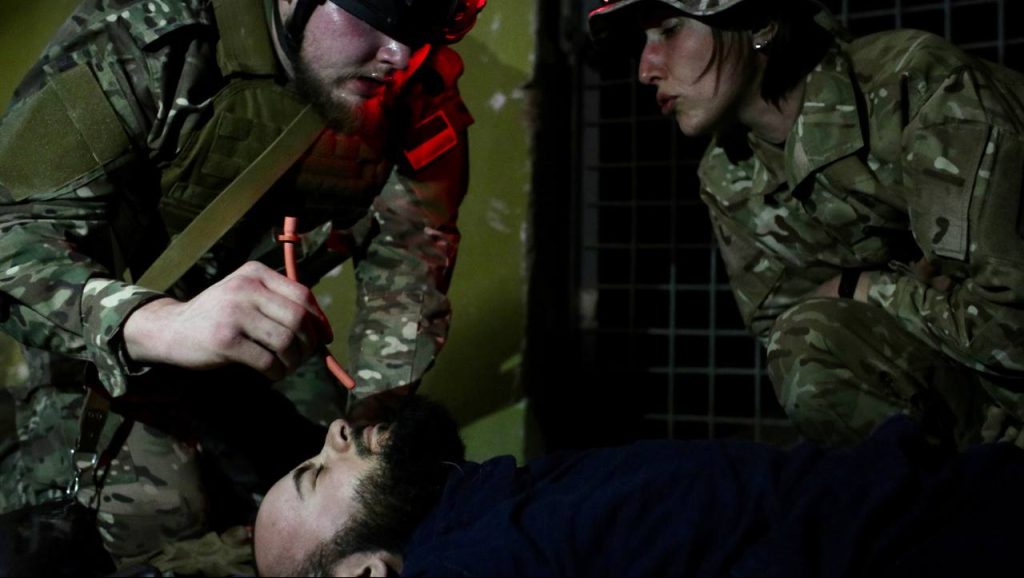
The Come Back Alive Foundation is deploying 8 mobile tactical medicine training complexes at training grounds in the north, south, east and west of Ukraine. It provides equipment, consumables and specialized property. It helps to train instructors according to a single standard approved by the Armed Forces. As a result, we have to create conditions for training about 200,000 military personnel a year in first aid according to the TCCC ASM level.
Liudmyla Pautets, head of the Come Back Alive tactical medicine instructor program, tells about her journey from a volunteer medic in the war to the Holding On project, which systematically strengthens the capacity of the Ukrainian army:
— I dreamed of being a doctor, but the education was too expensive. I chose healthcare management, which is cheaper and related to medicine. I wanted to work in hot spots, and I was very impressed by Medecins Sans Frontieres (Doctors Without Borders). But I needed work experience, so I got a job at a hospital. The salary was 900 hryvnias, “incompatible with life”. So I went into trade.
Doctors are like addicts — you want to quit medicine, but you can’t live without it. It’s always interesting. That’s why I came back. In Kyiv, I worked as an administrator and nurse in a private clinic, as well as in psychiatry on Kyrylivska Street. I also had two part-time jobs.
After the Maidan, when russia started its war against Ukraine, I went to the military registration and enlistment office and got a military ID. And decided to improve my knowledge. I found the Medsanbat project with foreign doctors. There I got acquainted with the TCCC (Tactical Combat Casualty Care) protocol. I studied, then assisted instructors and taught it myself.
In the summer of 2014, my friend was wounded in Donbas. He was a paratrooper, and in civilian life he was the director of the store where I used to work. I went with another friend to take him from Dnipropetrovs’k region to Odesa to have his broken nerve repaired. Back then, I was still hesitating whether I could help at the forefront. I wasn’t physically strong or resilient. “Small, thin and coughing.” How could I carry a wounded man on my back?
A piece of shrapnel hit his thigh. There was noone who knew how to provide first aid
Pavlo had no injuries of large vessels, but he lost more than three liters of blood. A piece of shrapnel hit his thigh. And there was no one who could provide first aid. They did not even apply a bandage. And he was just bleeding for several hours. If the injury had been more serious or the evacuation had taken longer, he would have died. So I realized that I would be useful in the war. And I started looking for the best place to go with my skills.

At the military enlistment office, I asked what to do if I signed a contract, what I would be provided with as a medic. They said I would have a week of training and go to the front. As for the rest, they didn’t give any answers. No, this didn’t work for me.
I thought about joining the Hospitallers or the Pravyi Sektor. I wanted to join Azov, but they did not accept women. There was a group of volunteers gathering after the Medsanbat course. I decided to be with them — we studied together, I was confident in their skills. I agreed with the team of the Separate Rapid Response Medical Brigade that I was going. And then the deputy commander came and said: no women. We were just in the parking lot near the Unimogs (Unimog Mercedes-Benz — a multifunctional four-wheel drive vehicle) we were supposed to work on. I knew German, and while we were arguing on the street, I looked at the labels on the cars and saw what they said. I said: “Come in, I’ll show you everything.” And they said then: “Well, maybe you’ll be useful.”
You have to look at the person, not the gender. How does it affect my work? Men are physically stronger, but they can also be frail. I have a year of experience in psychiatry, and I am mentally tough. I’m not afraid of blood and don’t panic in a critical situation. This is more important than being able to carry 200 kilograms. I decided to work with my brain and character.
I went to war with two sports bags and one checkered bag. I took a sterilizer, a stitcher, and sets of instruments
I bought myself a uniform, a backpack, and collected some medicine. I went to war with two sports bags and one checkered bag. I did not know what was waiting for us. I also took a sterilizer, a stitcher, and sets of instruments.
There were five regular medical crews and two resuscitation ambulances, where doctors took out very wounded patients on artificial ventilation devices, etc. My crew consisted of three people: me, a driver and a navigator, who helped me. We were all supervised by the chief medical officer of one of the brigades.
We stopped in Kostyantynivka. They turned the former psychiatric hospital into a warehouse. We were assigned to different areas. We had to go with the group to Stanytsia Luhanska. But then active battles for Donetsk airport began, its tower fell, and we had to urgently throw all our forces there.
We worked there until Debaltseve started. Then we were here and there, depending on the need. Our Unimog could accommodate several wounded people sitting or four lying down, and it saved a lot of time for evacuation and the number of accompanying personnel.
From the Donetsk airport, soldiers were taken to Karlivka mostly. There, we intercepted them and took them to the hospital in Selidove, Pokrovsk — then known as Krasnoarmiysk. There were serious shrapnel wounds, many contusions, and fractures. There were two or three cases of massive bleeding. Most of them were very exhausted fighters who sometimes hadn’t seen food for a week and hardly drank. They had been eating snow. The first time, we were so ashamed that we had no supplies with us. After that, we took tea in thermoses and food.
I remember my first wounded. We received him in Krasnoarmiysk. The guy had a broken hip. The doctor did not cut his pants. The bone fragment was sticking up a little bit, and when the doctor started taking them off, they rested against this protrusion and got stuck. He started pulling.
I rushed to cut the pants and saw two fused fragments in the groin area. If the doctor had pulled them out, they would have increased the bleeding. How can you treat a person like that? Some of the local doctors had separatist views. Later, we tried to control more, to take over the work in the reception area, so that the wounded were less uncomfortable.
We were supposed to work for two weeks. Two months later, I got home for a day
We were supposed to work in the combat zone two weeks after two weeks. But it happened that two months later I got home for a day. Then I came back and worked for another month, until the ceasefire after the withdrawal from Debaltseve (the fighting for the city ended on February 18, 2015. The Ukrainian military retreated in an organized manner — ed.)
I had my first heavy case in Debaltseve. We were transporting the wounded in two crews to Kramatorsk, and a helicopter picked us up from there. Our car got behind and got lost. The second crew was carrying a seriously wounded man in an ambulance. The helicopter would not take off until it was fully loaded. And the wounded man was already running out of oxygen on the ventilator. And in our car, a guy with a shrapnel wound to his shoulder and a damaged nerve was screaming frantically all the way. The car was shaking, and bone fragments were scratching his nerves. It became cold in the cabin, and the diesel level dropped. I took off my clothes and wrapped them up. We were driving to God-knows-where. The navigator didn’t work. I thought we would not get out alive.
We finally got there and loaded the wounded into the helicopter. It took a long time to move the heavy one, who was being transported by our guys on a resuscitation vehicle, because the stretcher got stuck. He ran out of oxygen. He was disconnected from the ventilator, and I started manually pumping him with an ambu bag. He began to regain consciousness. The anesthesia wore off, but he could not breathe on his own. I remember his facial expression, his eyes. His arm and leg were amputated. The pulling of the stretcher hurt him, and he could wake up from it. And I felt a lot of guilt afterwards. I kept going over in my head what could have been changed in that situation. I felt that my knowledge was not enough.
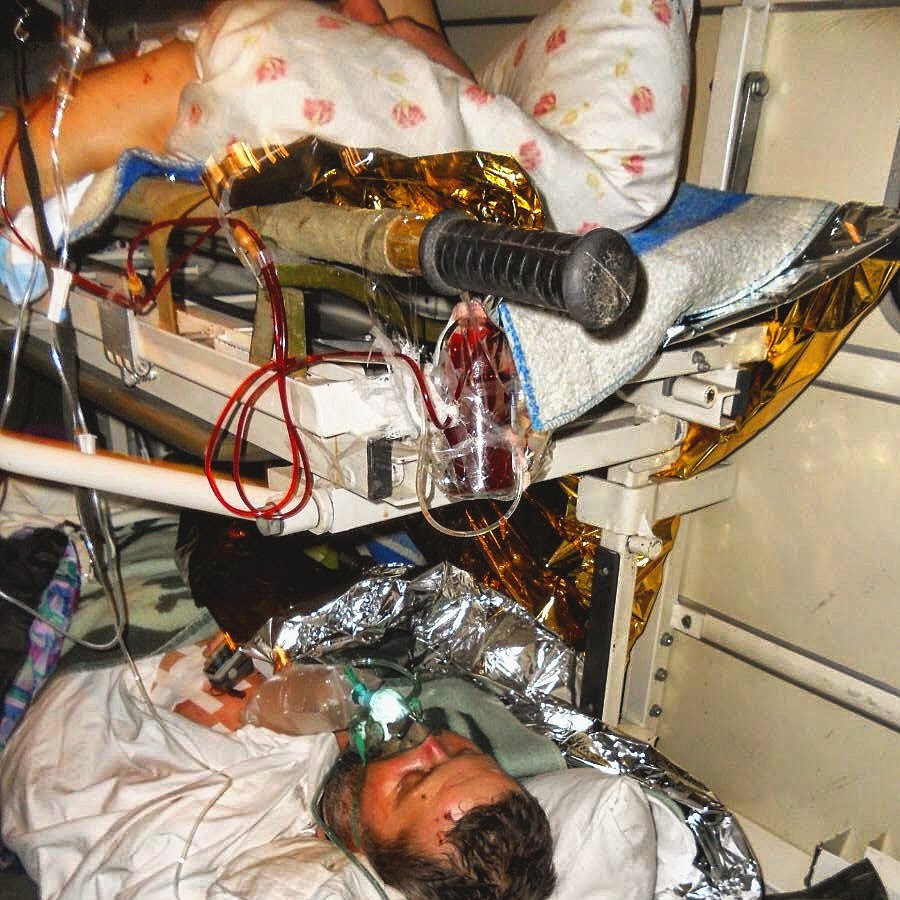
I learned about the ambu bag only at the Medsanbat courses. I was a nurse, but no one showed us this. We were taught how to assemble and disassemble glass syringes, and we were taught from Soviet books. What knowledge did they give me, what can I do? To give an injection, to measure blood pressure. And in combat conditions, what can you do with that? After that, I took all possible courses that appeared in Ukraine.
A medic found a survivor among the dead when he was reloading bodies – he heard breathing, heartbeat
The intensity of fighting decreased. And in April, between evacuations, we started to teach the military more about first aid in the frontline areas where we worked. We came to hospitals and stabilization centers and conducted short courses. At least how to use a tourniquet, apply bandages — some primitive things to help the wounded survive until the arrival of a doctor. We also invited medics from neighboring units, riflemen, medics, who were often people with no knowledge at all: “Here’s a bag of medicines for you to sort out.”
Sometimes the military could not even determine whether a person was alive. They did not know how to check the pulse or pupil reaction. During the battles for Debaltseve, a medic found a man alive among the dead when he was reloading bodies. He checked for signs of life and heard breathing and heartbeat.
They poured sugar into the wound, poured calcium chloride, stuffed chewed moss with salt, tamponaded it with bread, and covered it with egg white
The soldiers had absolutely no knowledge then. Some were told something by the Afghans, others read something somewhere. They poured sugar into the wound, poured calcium chloride, stuffed chewed moss with salt, tamponaded it with bread, and covered it with egg white. Now the awareness, even with all the problems, is incomparable.
Teaching is not my thing. I love practice. But I realized that I can do less on my own than all those with whom I share information.
Once we trained a unit, and a week and a half or two weeks later, a fighter was wounded. The former cadets did a great job and saved him. His commander gave me a cool, expensive stretcher as a thank you, which was impossible to find in Ukraine.
The first thing in medicine is to do no harm. I was very afraid of doing something wrong. One case haunted me for a long time. There was a severe injury — two shrapnel fragments in the head. Such cases were always treated by the medical team. But the doctor had an even more severely wounded fighter. And the doctor said that I should take him to the hospital by myself. He said a paramedic would come with us to help. The guy was injected with drugs that lower blood pressure so that the cranial hematoma would not grow. And we are driving along the road, which is shot up, and I can’t feel the pulse. We stop, I measure his blood pressure — 20 over 0. If we don’t raise it, his heart will stop, and if we raise it, a hematoma may grow and he will die. I did not work in intensive care and did not have the knowledge of what to do in such a situation.
Holding a bag with the remains of his combat brother. He is worried whether the remains are enough for DNA analysis
We are standing not far from the checkpoint, and we can already see nervous movements there — we are coming from the enemy’s side. The driver knocks: hurry up. I went to the paramedic and he was out of it. He is holding a bag with the remains of a fellow soldier who was killed by a direct hit. He had to collect what was left of him. He is worried whether the remains are enough for DNA analysis. I realize that he will not help. I could not get through to the doctor who handed over the wounded man to me. I decided to take responsibility and raised the pressure. We brought him to a neurosurgeon. But I kept thinking later what happened to him, whether he was able to recover. But in that situation, with the knowledge I had, I couldn’t do anything better.
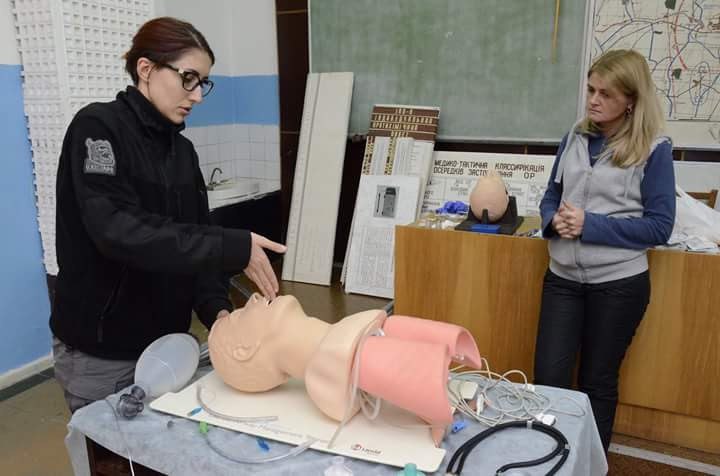
At the All-Ukrainian Resuscitation Council in Dnipro, I took two TCCC training courses. And I asked to become an instructor – I was the first person they gave this certificate to. Until then, my knowledge was a hodgepodge. And here I saw the structure and methodology of teaching: you have to talk about a skill, such as putting up a tourniquet, and do it clearly. I liked it. I realized that I needed to learn from people who think systematically.
In 2015, police training began according to new standards, and I was invited to teach tactical medicine. Later, my comrades and I decided to assemble an instructor group and organize TacCat, a first aid course based on officially recognized protocols for both military and civilians.
They taught bleeding control, basic life support, and assistance in tactical conditions. They received certification and, based on this knowledge, could develop their own courses, for example, on road accident care. We were struck by the fact that in the first two years of the war, more people died on the roads than at the front. We decided to do something about it. We even managed to make some changes to the driving school programs.
About 5,000 people took our training courses. We had a feeling that knowledge of tactical medicine should be disseminated on a large scale.
We tried to popularize it. To make it interesting, even fashionable. You get knowledge, extreme – even if you work with artificial blood, your hands shake. In addition, working with simulators and realistic models of wounds gives you emotions that help you retain what you have learned better in your memory. People shared their enthusiasm and encouraged others to come to the course: it’s hard, but it’s cool. Due to the covid pandemic, the project had to be put on hold.
Here’s the address of the pharmacy, take the key under a rock, and take everything out where it’s needed
During the first weeks of the full-scale invasion, while there was no foreign volunteer help, I traveled with my colleagues in Kyiv to collect medicines and send them to units, hospitals, and clinics. They would call me and say: “Here’s the address of the pharmacy, take the key under a rock, take everything out where it’s needed.” We made backpacks for medics, sewed pouches out of jeans because there was nowhere to pack individual first aid kits. People made turnstiles out of curlers and pieces of fabric, and all the supplies, even training ones, were distributed.
We shared with our colleagues from Motohelp, Hospitallers and others the areas of responsibility in and around the capital. Ours was Irpin, the bridge to Romanivka, Zhulyany airport.
In Solomianka, there was a volunteer hospital in a private clinic, with evacuation teams. We started training them in TCCC. The military and rescuers also came to the trainings. During the storming of Nova Kakhovka, one of our cadets had a piece of his leg torn off. I watched the video – the first aid was almost perfect. When I see this, I think that I have not lived in vain.

In 2022, the nature of war injuries changed. Previously, there were close shooting battles, but now they are bombing with anything. Shrapnel comes from different directions and even hits parts of the body under body armor. There were much fewer torso wounds. But the survival rate after them has also increased. Our medics are already skilled in their work. If in 2014 a person could die from a simple bullet wound to the shin, nowadays people with very serious injuries survive and recover.
We got a head start at the expense of the ATO/JFO. If there had been a full-scale invasion at once, there would have been much more casualties. During the 8 years of war, many active people have learned how to provide assistance properly, regardless of civilian or military protocol. Blood flows the same way, bandages are applied, splints are applied – no matter what the injury is.
Changes were often initiated by activists and volunteers from outside
With the medical reform, the primary level of care, emergency care, and paramedics appeared. In the army, it was a matter of luck. The chief medical officer could teach first aid from a book on pre-conscription training for young men, using methods from the Second World War. At the same time, a medical company was created at the 169th training center in Desna and the 205th training center for tactical medicine. Changes were often initiated by activists and volunteers from outside.
Last summer, the Armed Forces approved the transition to a single standard of first aid, the Alliance’s TCCC. Volunteers and activists helped. They translated all the materials, videos, and presentations. They are freely available, but you need to understand how to teach, how to organize the educational process accordingly.
The American TCCC ASM (All Service Members Course — a standard for providing pre-hospital care on the battlefield, developed for all military personnel who are not medics — ed.) is used by most developed countries. It shows effectiveness, reducing mortality from 27% to 3% in some units. It all depends on how long and to what level the unit trains first aid.
This standard is logical and has simple acronyms that are easy to learn. For example, MARCH (an algorithm that determines the priorities and order of actions in helping the wounded: massive bleeding, airways, respiration, circulation, head injury/ hypothermia).
We interacted with the Medical Forces Command of the Armed Forces of Ukraine, the Military Medical Academy, and helped with training programs
We had been preparing the launch of the Holding On project for four months. We interacted with the Medical Forces Command of the Armed Forces of Ukraine, the Military Medical Academy, and helped with training programs. We traveled to each of the 8 training grounds where we deploy training centers. We found out how many instructors they have on staff, when they were recruited, and how they are trained. What program do they teach, does it meet the requirements? How many more people can they hire?
We also worked with non-governmental organizations that provide training and certification. We brought them together in a single database so that we could attract their volunteers to the training grounds.
We are sending 96 range instructors to the 184th training center. There they are trained as ASM instructors. They are taught how to teach this 8-hour course as part of basic military training. They receive a presentation, an outline, and return to their training grounds to work on the new program.
If an instructor fails to pass the training, he or she is expelled from the course. If he fails to fulfill his duties and is not certified, we recommend that the range management replace him.
When we already have trained instructors at the training ground, we set up a tent with all the equipment — chairs, projectors, screens, speakers, and mannequins. Previously, many of them taught tactical medicine right in the forest on the ground, even in winter. Some had tents without floors, lighting, or heating. Under such conditions, the quality of information acquisition was minimal.
We want to increase the number of centers where instructors can be trained
Next, we will monitor how training centers change and implement programs. And we want to increase the number of centers where instructors can be trained.
We are not giving them a fish, but a fishing rod. Instead of teaching tactics to soldiers ourselves, we help the army to do it efficiently and on a large scale. We are running out of time. We need to do everything by yesterday. Especially before the counteroffensive, we need to train as many people as possible.
Join the fundraiser for the “Holding On” project
More on topic
Online course for drone operators launched
30 Nov 2022, 15:00
«Сome Back Alive» purchased 11 armored vehicles for the 36th Marine Brigade
08 Sep 2022, 07:26


